Data science has transitioned from experimental hype to governed, operational deployment across the healthcare industry. In 2026, the technology is no longer discussed in terms of “future potential” but as a current standard of care, driven by stringent interoperability requirements, clinical workflow integration, and human-in-the-loop oversight. With over 80% of physicians now using AI professionally and the global healthcare analytics market projected for sustained expansion, value is created at the intersection of high-quality data, robust governance, and proven clinical workflows.
This article examines where data science already delivers measurable impact in diagnostics, hospital operations, personalized treatment, and pharmaceutical development. We will explore concrete use cases, outline the conditions that separate successful implementations from failed pilots, and share verified case studies. If you want to evaluate how these applications of data map to your infrastructure, schedule a call.
What is Data Science in the Healthcare Industry?
Data science uses advanced analytics, machine learning, and artificial intelligence to uncover previously hidden patterns within large amounts of data. Applying data science in healthcare and medicine can use predictive algorithms to derive insights and make predictions that improve patient outcomes. It includes predictive analytics and image analysis—which help identify patterns that would be impossible to detect with other methods. Health, medical, and biomedical data science are all branches of the larger field of data analytics. This data can include electronic health records, medical imaging, and other sources of healthcare-related information. Some examples of how data science is currently used in healthcare include predicting patient readmissions and identifying patients at risk for developing chronic diseases. Additionally, the practice has been proven to enhance the accuracy of medical diagnoses.
Overview of the Healthcare Industry
In recent years, according to research by Springer in the healthcare industry, data science has become increasingly important due to the vast amounts of data generated from patient records, medical images, and clinical trial results. Healthcare organizations can use these methodologies, powered by advanced analytics and machine learning, to make sense of the data they collect and apply it to improve patient outcomes, optimize operations, and cut costs.
For example, Predictive analytics can help healthcare providers identify patients at risk for certain conditions and intervene early—preventing the condition from progressing. Precision medicine tailors treatment plans to individual patients based on their unique genetic makeup and other factors.
DATAFOREST specializes in helping healthcare organizations implement solutions that harness the power of Data Science. Our team can develop and deploy data-driven strategies to improve patient outcomes, streamline operations, and drive business success. See more... about how we found the solution for similar performance challenges.
Advantages of Data Science in Healthcare
The global healthcare analytics market size is expected to reach USD 167.0 billion by 2030, expanding at a CAGR of 21.4% during the forecast period, according to a new report by Grand View Research Inc. This massive growth reflects how health data science, or health informatics, delivers tangible value across clinical and operational functions.
Here are 10 key benefits of data science for healthcare organizations:
- Improved patient outcomes: Data science can help healthcare providers develop more effective treatment plans by considering individual patient data.
- Predictive analytics: National Library of Medicine discusses a survey that used machine learning approaches to predict diabetes risk, demonstrating how early risk flagging prevents disease progression.
- Precision medicine: By using data science to tailor treatment plans, doctors can make better decisions about how best to treat individual patients.
- Enhanced research: Data science is an emerging field that uses large datasets, combined with machine learning, to identify patterns and trends relevant to medical research. It can lead to the discovery of new treatments.
- Operational optimization: Research by Harvard Business Review demonstrated the potential of data analytics in optimizing hospital staff scheduling, reducing burnout and improving care continuity.
- Improved patient engagement: Personalized data analysis can help healthcare providers understand their patients better, improving adherence and outcomes.
- Real-time monitoring: Healthcare providers can use data science to monitor patient health in real-time, improving outcomes and the timing of interventions.
- Cost reduction: Scientific Reports used machine learning to predict the hospital readmission risk from patients' claims data using machine learning, proving that early intervention significantly lowers costly readmissions.
- Improved decision-making: Data-driven decision-making helps organizations understand population health trends and improve outcomes while reducing operational waste.
- Better resource allocation: Data analysis can help healthcare organizations make better decisions about how to spend money and provide high-quality care. With proper data science tools, hospitals can allocate beds, staff, and equipment more effectively.
Book a call to discuss how these benefits can apply to your organization.
How Data Science Can Improve Healthcare Systems
Data science significantly impacts the healthcare industry, helping organizations improve patient outcomes and drive innovation. Healthcare providers can use data analytics models to make more effective decisions, identify areas for improvement and develop better treatment plans.
Data science can also help healthcare organizations stay up-to-date with the latest research and developments, leading to more effective treatments and interventions. This will ultimately improve patient care by delivering more efficient services and personalized medicine options across multiple stages, from diagnostic tests to treatment recovery. Learn more about data science in healthcare and how it reshapes care delivery.
Healthcare companies can use data science to allocate resources more efficiently and effectively, reducing costs while improving profitability. As healthcare becomes less about treatment for illness or injury and more about prevention of disease, the importance of using data science to understand patients better will continue to grow.
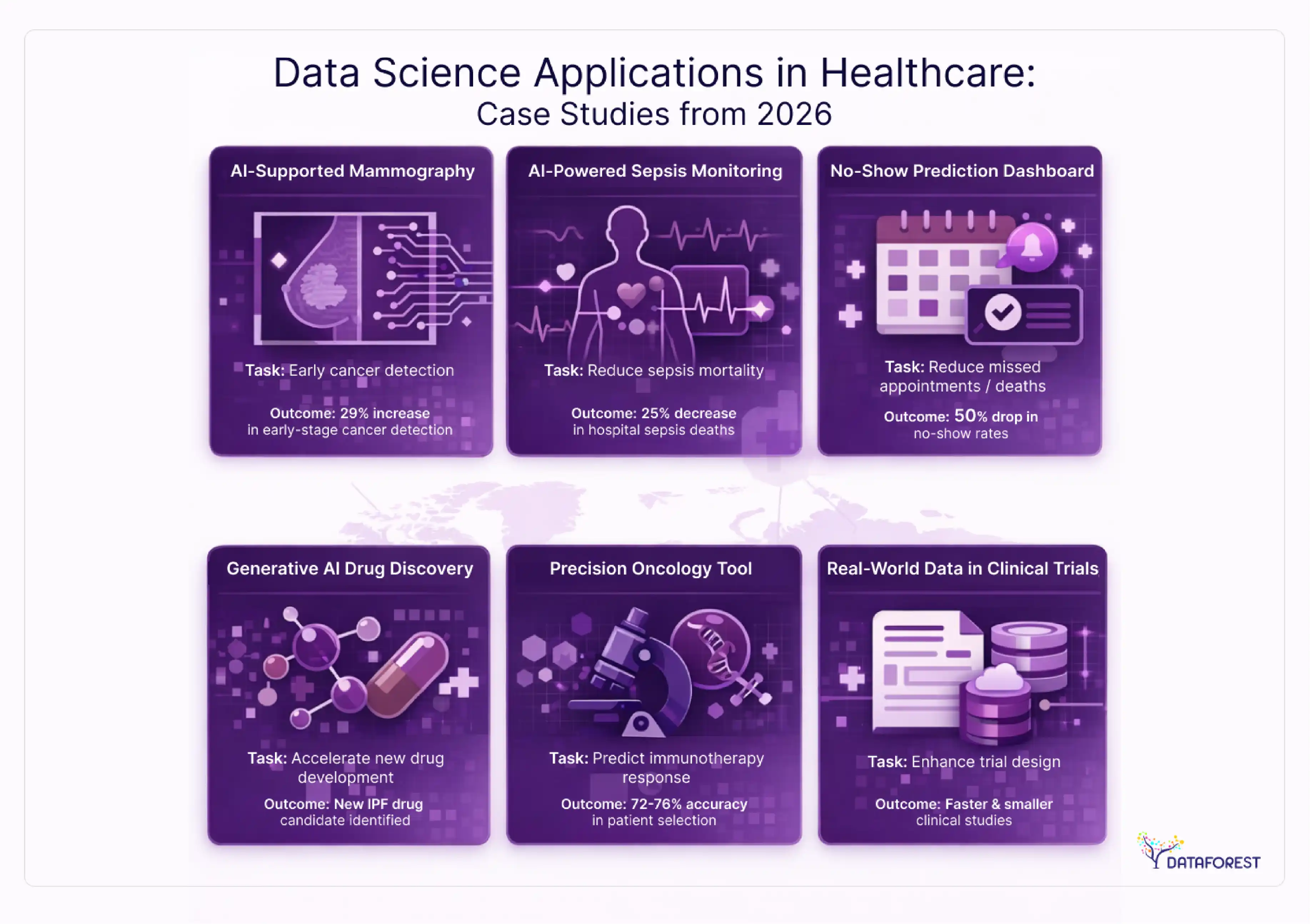
Data Science Applications in Healthcare Industry: Case Studies
Data science has become an essential tool in the healthcare industry, as technology makes it easier to collect and analyze large amounts of data. Below are verified 2026 implementations that demonstrate measurable outcomes.
1. AI-Supported Mammography Screening (Diagnostics)
Task: Reduce workload for radiologists while improving early detection rates without increasing false positives.
Approach: Integration of a deep learning model into routine mammography screening workflows, validated through the MASAI trial framework. The system acts as a decision-support layer, prioritizing high-suspicion cases for rapid review.
Outcome: The AI-assisted workflow demonstrated a 12% reduction in interval cancer diagnoses, a 44% decrease in radiologist reading workload, and a 29% increase in early-stage cancer detection without raising false-positive rates. Advanced cancers were identified earlier, improving treatment trajectories.
Why it matters: Proves that AI in diagnostics delivers value not just through image recognition, but when embedded into safe, clinically supervised workflows that balance workforce efficiency with diagnostic precision.
2. AI-Powered Sepsis Learning Health System (Quality of Care)
Task: Reduce in-hospital and post-discharge sepsis mortality through real-time risk flagging and standardized care pathways.
Approach: Deployment of a continuous learning health system across 97,559 patient stays at a major university hospital. The HERACLES AI model continuously monitors vital signs, labs, and EHR data, triggering a clinical dashboard and protocolized antibiotic administration when risk thresholds are crossed.
Outcome: For AI-flagged sepsis cases, in-hospital mortality dropped from 20.54% to 15.27%, and 90-day mortality fell from 32.99% to 26.11%. Protocol compliance increased, leading to faster time-to-antibiotics.
Why it matters: Highlights that value comes from a closed-loop system combining predictive modeling, human oversight, and integrated clinical pathways—not from standalone algorithms.
3. Real-Time Dashboard for No-Show Reduction & Patient Flow (Operations)
Task: Optimize clinic scheduling and reduce appointment no-show rates in primary care.
Approach: Implementation of an AI-driven prediction model coupled with a real-time operational dashboard analyzing historical attendance, demographic, and booking pattern data across 135,393 appointments. The system auto-generates optimized slot allocations and targeted patient reminders.
Outcome: Achieved an 86% prediction accuracy for no-shows, resulting in a 50.7% reduction in missed appointments. Average patient wait times decreased by 5.7 minutes, with high-volume clinics seeing up to 50% wait-time reductions.
Why it matters: Translates operational data directly into capacity optimization, staff efficiency, and improved patient experience with clear ROI metrics.
4. Generative AI in Drug Discovery (Rentosertib for IPF)
Task: Accelerate identification and clinical validation of novel drug candidates for idiopathic pulmonary fibrosis.
Approach: Utilization of a generative AI workflow to identify biological targets and design novel molecular structures. This aligns with regulatory frameworks outlined in The FDA's discussion papers on the use of AI and ML in drug development and manufacturing. The pipeline prioritized compounds with high predicted efficacy and favorable pharmacokinetic profiles, moving rapidly into phase 2a randomized trials.
Outcome: Successful validation of rentosertib, a first-in-class TNIK inhibitor, with the model directly informing target selection and lead optimization. Regulatory and editorial analyses recognize this as a concrete clinical milestone for AI-enabled drug discovery.
Why it matters: Demonstrates that AI in pharma has moved from theoretical screening to tangible clinical pipeline acceleration, reducing early-stage R&D friction and costs.
5. Precision Oncology: Predicting Immunotherapy Response (SCORPIO)
Task: Improve patient selection for immune checkpoint inhibitor therapy, which traditionally benefits only a subset of patients.
Approach: The SCORPIO tool analyzes routine blood tests combined with electronic medical records across nearly 10,000 patients and 21 cancer types. Supported by foundational research in Big Data in Basic and Translational Cancer Research and the broader use of big data in oncology, machine learning models identify complex biomarker interactions to predict therapy response and overall survival.
Outcome: As noted in the review article published in nature provides insights into the progress made by scientists in using machine learning to predict patients' responses to medications, SCORPIO achieved 72%–76% predictive performance across validation cohorts, outperforming several standard FDA-approved diagnostic tests in forecasting response and survival outcomes.
Why it matters: Shifts personalized oncology from broad genetic matching to accessible, data-driven treatment stratification, reducing adverse events and optimizing high-cost immunotherapy allocation.
6. Real-World Evidence & External Controls in Clinical Development
Task: Enhance clinical trial design by supplementing randomized control arms with high-quality historical and real-world patient data.
Approach: Integration of structured real-world datasets into trial simulation frameworks, reflecting modern perspectives on the Role of Data Analytics in Improving Clinical Trials and Drug Discovery. Data pipelines enforce strict provenance, bias mitigation, and endpoint harmonization.
Outcome: While not a single deployment, this strategic application is actively reshaping trial architecture in 2026. Organizations leveraging validated external controls report faster patient stratification, smaller required sample sizes for rare diseases, and stronger post-market evidence continuity.
Why it matters: Shows that data science is transforming clinical development from a purely experimental framework into an evidence-generation ecosystem, provided regulatory and methodological rigor is maintained. Analytics for clinical trials is a key differentiator here.
Challenges and Limitations of Data Science in Healthcare
Using data science in healthcare projects has immense potential to transform the industry. However, several challenges and limitations must be addressed to realize its full benefits. If you need an individual approach to a solution, book a call.
Data Privacy and Security
Patient information is confidential and should be treated as such. Unauthorized access or disclosure of this data could lead to identity theft, financial loss, and damage to a healthcare provider's reputation. Healthcare providers must implement robust data privacy and security measures to protect patient data. Encryption can protect data in transit and at rest while limiting access to authorized personnel only. Multi-factor authentication is another important measure that an organization can implement.
Limited Availability of Data
Accurate and comprehensive data is essential for effective healthcare decision-making, but various challenges limit access to this data. These include silos where different parts of the system are separated; interoperability issues that make it hard for programs to communicate; and lack of standardization—where processes vary significantly between organizations or even within the same organization, depending on who's doing what. Healthcare providers and data science companies must work together to address these challenges to ensure that patient health records are reliable and up-to-date.
Technical Challenges
Providing patients with the best possible care is a top priority. However, achieving this goal requires more than skilled staff and advanced equipment. It also requires effectively managing and sharing large amounts of data generated by electronic medical records (EMRs). Unfortunately, many healthcare providers struggle with sharing data due to outdated technology infrastructure and legacy systems. Healthcare providers must invest in modern technology infrastructure and data management systems to overcome these challenges. By partnering with established experts like DATAFOREST, providers can gain the necessary technical stacks and architectural guidance to implement advanced, compliant data management systems.
Ethical and Governance Considerations
Finally, data science in healthcare raises ethical and regulatory considerations. Beyond basic privacy and consent, 2026 deployments must address model transparency, lifecycle management, post-market monitoring, and human oversight. WHO guidance and updated FDA frameworks emphasize that AI-enabled systems require continuous validation, bias mitigation, and clear accountability structures. Healthcare providers and data science companies must meet these strict standards, obtain informed consent where applicable, and ensure models are deployed for legitimate, transparent clinical purposes only. Book a consultation to map out a compliant deployment path.
Future of Data Science in Healthcare
Technological innovations and the emergence of new methods
Advances in technology and techniques are opening up new avenues for data science in healthcare. AI algorithms and machine learning programs can now analyze large datasets to provide more sophisticated analysis than ever before. Natural language processing (NLP) is increasing, making it possible to analyze unstructured data such as physician notes and patient narratives. In addition, data sources such as wearable devices and remote patient monitoring technologies are becoming available, providing real-time health information for more personalized treatment regimens.
How Data Science Can Be Used to Further Clinical Practice
The future of data science in healthcare is to make it a part of everyday medical practice, using data-driven insights to improve patient outcomes. Predictive models can identify patients at high risk of developing certain diseases or conditions—helping doctors make decisions about early intervention. Data science can help make healthcare more efficient and less expensive by identifying patients at risk for hospital readmission and intervening to lower those risks.
Impact on Healthcare Outcomes
Data science can improve healthcare outcomes by enabling early intervention, tailoring treatments to individual characteristics, and streamlining care delivery. This leads to improved efficiency and reduced costs—essential goals that every hospital strives to achieve, and a core driver behind transforming healthcare.
How Data Scientists Can Work with Healthcare Professionals
Healthcare data scientists and medical staff must collaborate closely. Healthcare professionals provide the domain expertise to interpret findings in clinical context, while data scientists build scalable pipelines, validate models, and deploy analytical tools. This partnership enables truly personalized and evidence-based care.
Summary of Key Points
- The healthcare industry is constantly evolving, facing new challenges such as changing regulations, technological advances, and shifting patient needs—but also great opportunities.
- Patient-centered care should be prioritized, involving patients in decision-making and tailoring treatments to individual needs.
- We must embrace technology such as electronic health records and telemedicine to improve efficiency, accuracy, and patient outcomes.
- The industry must address rising demand for preventive care, alongside issues related to access and affordability.
- Quality and safety must remain central, especially in medication delivery, infection control, and patient education.
Implications for Healthcare Industry & Conclusion
Healthcare's increasing use of data science has significant implications for the industry. By leveraging structured and unstructured data, healthcare providers and pharmaceutical companies can improve patient outcomes while reducing costs—and accelerating drug discovery. Using data science to support the drug discovery and development process has the potential to significantly reduce timelines, leading to faster market entry for innovative therapies. Personalized medicine, powered by predictive biomarkers, optimizes high-cost treatment allocation and reduces adverse events.
In 2026, the competitive advantage in healthcare no longer belongs to organizations that simply adopt AI, but to those that successfully integrate analytics and data science into clinical and operational workflows, backed by strong data governance, interoperability, and human oversight. The question is no longer “should we implement data science,” but “which use cases deliver measurable ROI, and do our data foundations, compliance frameworks, and staff readiness support sustainable deployment?”
At DATAFOREST, we specialize in providing custom data-driven solutions for healthcare organizations. We help teams move from pilot concepts to production-ready systems, focusing on feasibility assessment, data readiness, workflow integration, and measurable clinical outcomes. If you are ready to evaluate your use cases or explore our specialized healthcare analytics services, we'd be happy to talk with you about how we can address your unique Data Science challenges.
FAQ
What is data science, and how can data science be used in healthcare?
Data science is the practice of extracting insights and knowledge from data. In healthcare, it involves using statistical and computational methods to analyze health data, such as electronic health records, medical imaging, and clinical trials. This information can be used to improve patient outcomes, optimize healthcare operations, and develop new treatments.
What are some examples of how to use data science in healthcare?
Data science has been used to predict disease outbreaks, develop personalized treatment plans, and identify high-risk patients who require early intervention. For example, machine learning algorithms have been used to analyze medical images and identify early signs of cancer, leading to earlier detection and improved survival rates.
What are the challenges and limitations for healthcare data scientists?
Data scientists working with healthcare data often face data quality, privacy, and security challenges. Healthcare data is often complex, fragmented, and difficult to access across legacy systems. Additionally, strict regulations around the use and sharing of patient data can limit the types of analyses that can be performed without explicit compliance frameworks.
What ethical issues must be considered when using data science in healthcare?
Ethical considerations include ensuring patient privacy, obtaining informed consent, and actively mitigating algorithmic bias. It is essential to use data responsibly, prioritize model transparency and lifecycle monitoring, and ensure clinical accountability and patient welfare above all else.
What impact can data science have on drug discovery and development?
Data science can identify new drug targets, predict drug efficacy and toxicity, and optimize clinical trial design. By leveraging large-scale data analysis and generative workflows, it accelerates the development pipeline, reduces R&D costs, and brings novel therapies to patients faster.
How does data science affect healthcare operations and staffing?
Data science can help healthcare organizations optimize staffing levels, reduce wait times, and improve patient flow. By analyzing operational data, such as patient census and appointment schedules, data science can help healthcare organizations make data-driven decisions and improve overall efficiency.
How can healthcare professionals and data scientists collaborate effectively?
Effective collaboration requires clear communication, shared terminology, and a mutual commitment to clinical value and patient safety. Clinicians provide real-world context, ethical boundaries, and outcome validation, while data scientists ensure robust architecture, reproducible modeling, and seamless EHR integration. Together, they build solutions that are both technically sound and clinically actionable.





.svg)








